What if you could guarantee revenue integrity and clinical compliance on every chart?
Charta is the AI chart review platform that delivers 11% revenue uplift by scaling pre-billing chart review across 100% of patient encounters.
Member of healthcare organizations like






Strengthen coding accuracy, documentation compliance, and clinical quality
Charta builds AI chart review solutions for organizations across the healthcare ecosystem. Our AI engineers customize every integration to achieve the unique goals of provider organizations, health systems, payers, MSOs, and other industry stakeholders.
Instant, accurate codes for every encounter
Charta reviews all documentation immediately after note submission to completely and accurately code every service.
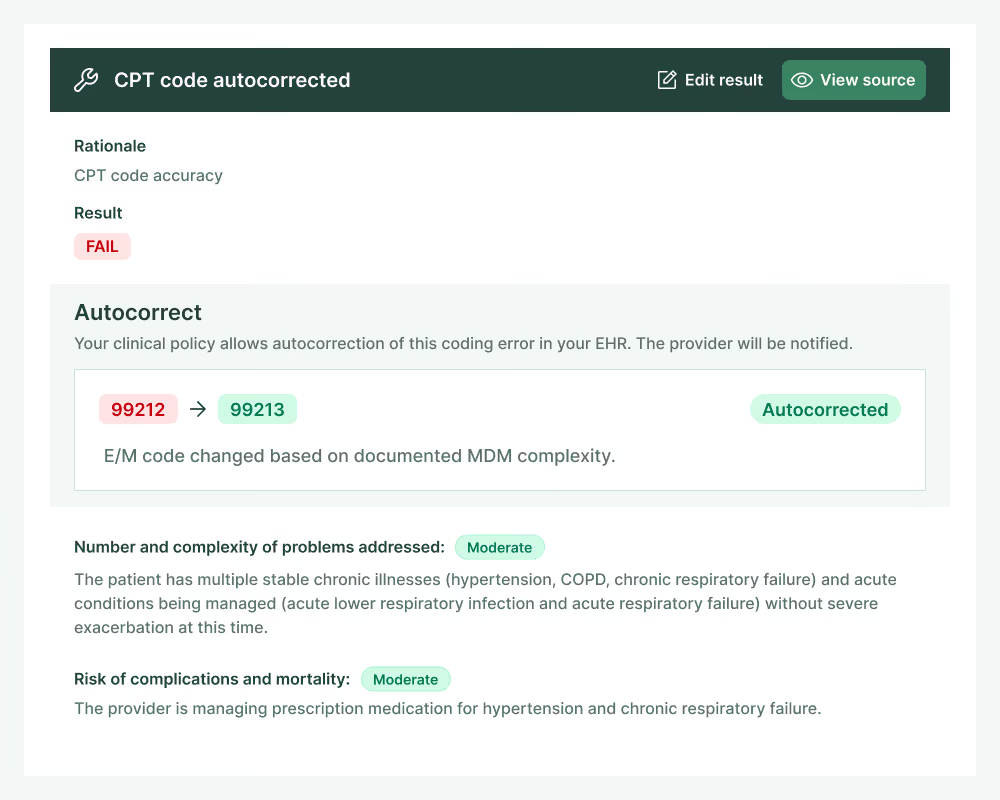
End coding-related revenue leaks
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.

Get peace of mind and greater control
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.

Real-time provider feedback
Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.

Higher ROI and greater insights into risk adjustment
Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.

Autonomous coding
Instant, accurate codes for every encounter
Charta reviews all documentation immediately after note submission to completely and accurately code every service.
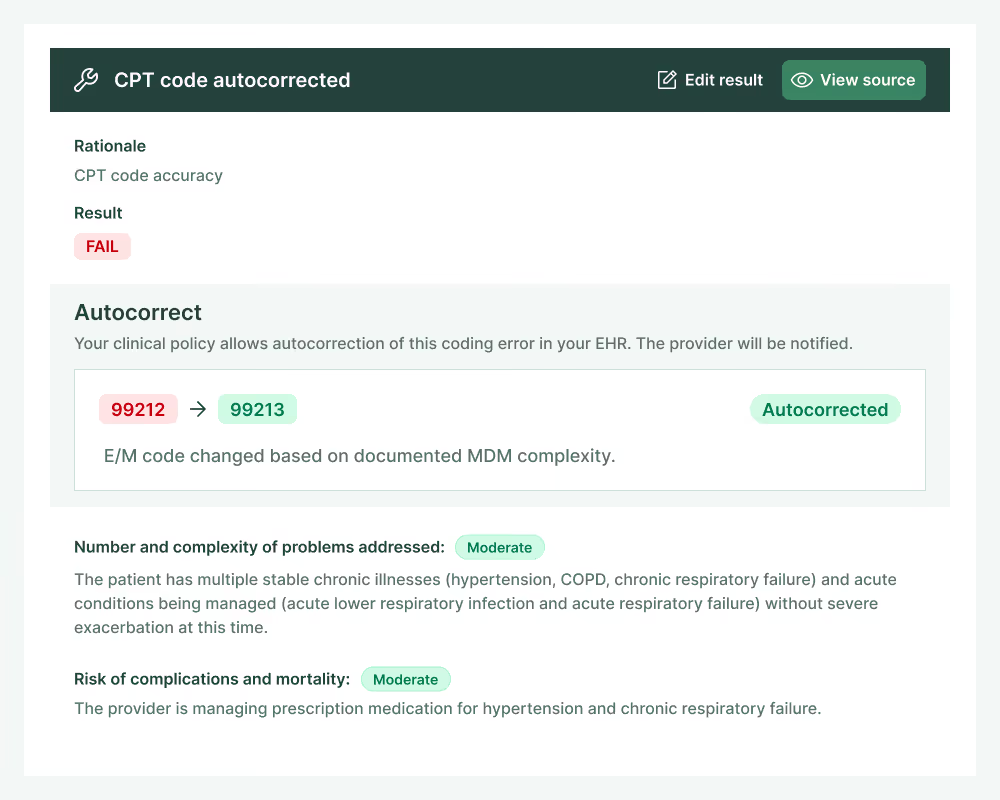
Revenue discovery
End coding-related revenue leaks
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.
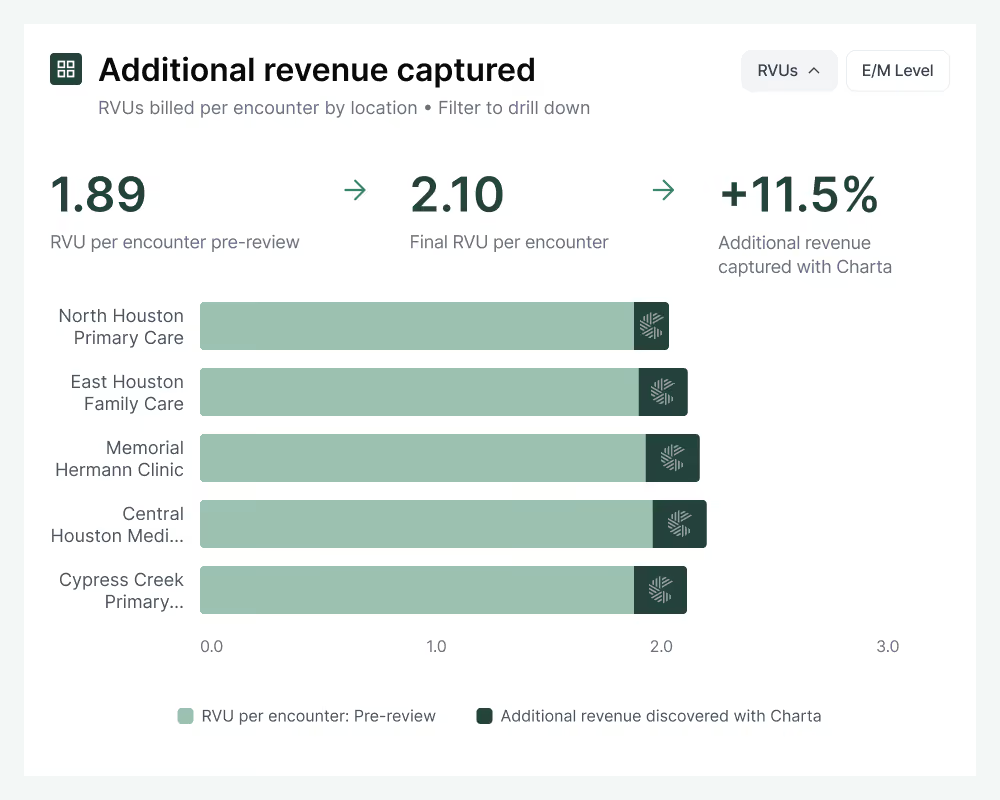
Payer compliance
Get peace of mind and greater control
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.
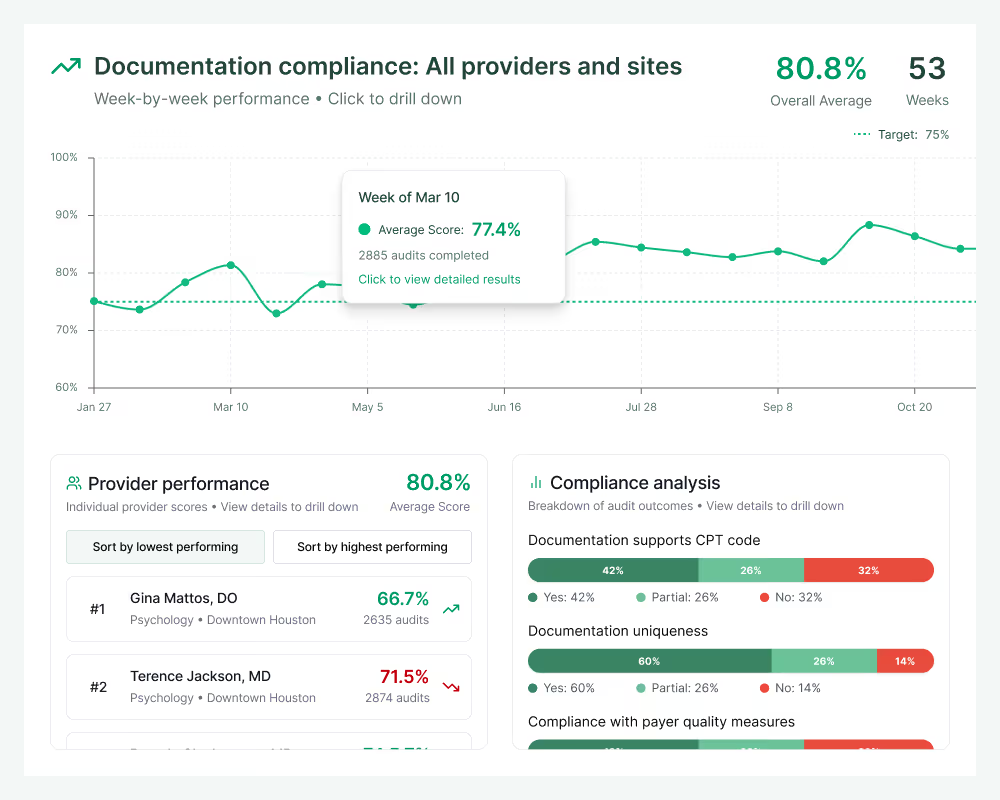
Clinical quality
Real-time provider feedback
Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.
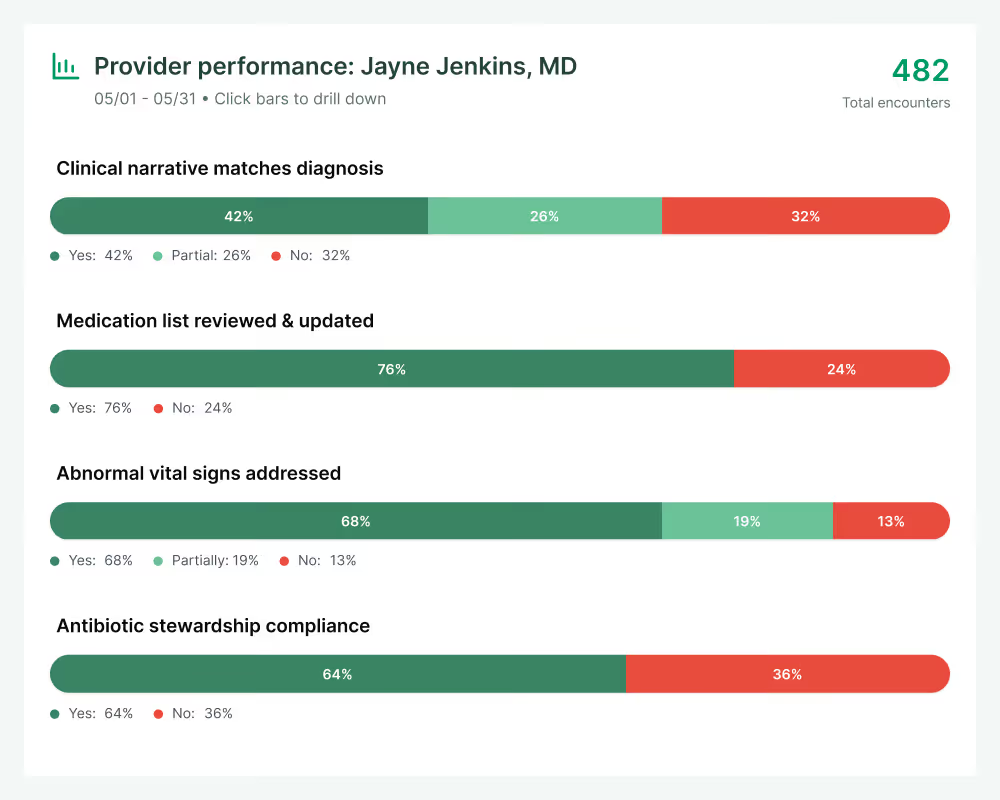
Risk adjustment
Higher ROI and greater insights into risk adjustment
Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.
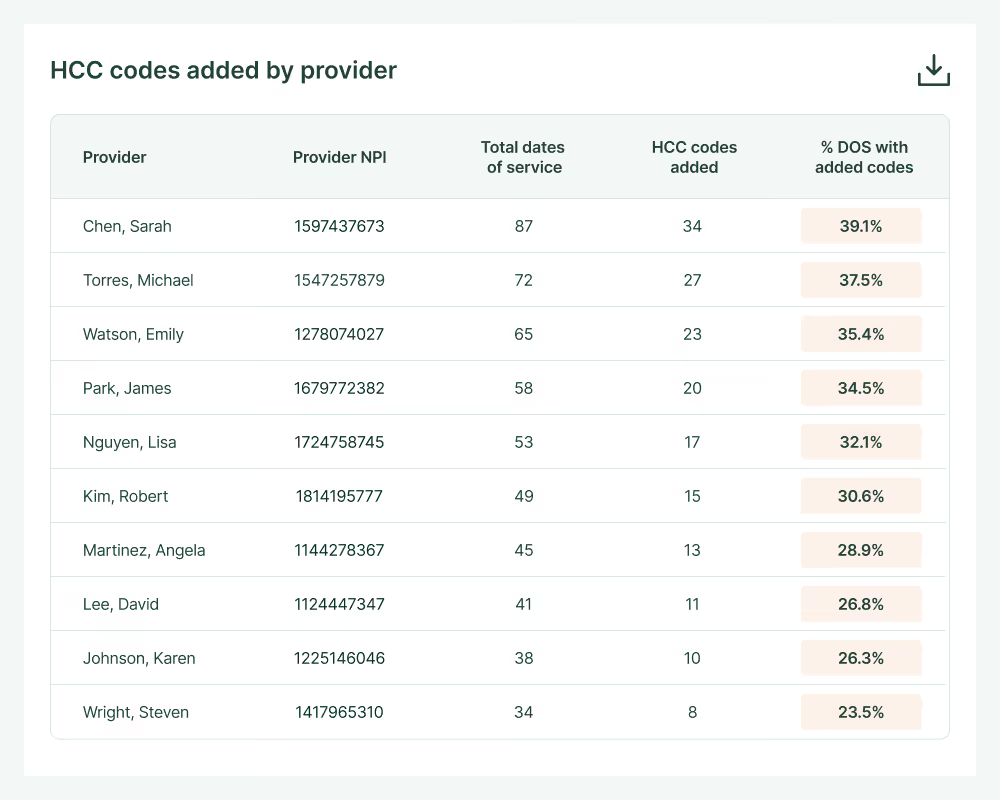
Built for teams across your practice
Provider organizations use Charta to increase capture revenue and build scalable systems for payer compliance, physician performance management, and clinical quality assurance. Browse solutions by role below.
How Charta works
Charta partners with provider groups, payers, MSOs, and other healthcare organizations to build customized AI models and data dashboards for comprehensive chart analysis across providers and sites.
01. Customized EHR integration
Charta integrates directly with your EHR. Your Charta engineer will build a customized integration that responds to the workflows and capabilities that your teams are already using.
Following implementation, you’ll retain access to your dedicated Charta engineer, who can adjust your model based on new payer and CMS rules, new state guidelines, provider feedback, and any other recommendations from your team.
02. Automated pre-billing chart audits
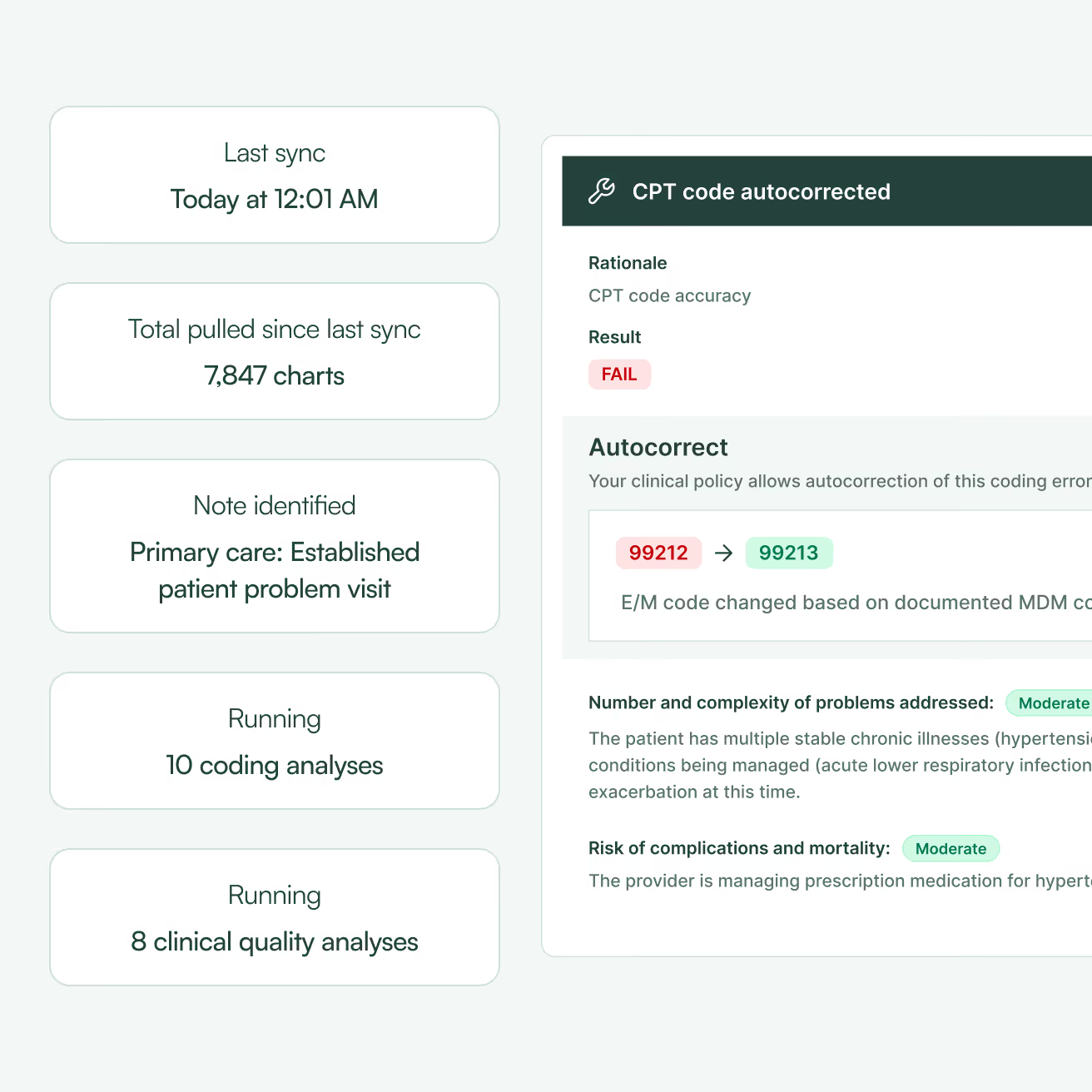
Every time a provider closes a note in your EHR, Charta identifies the encounter type and runs the analysis modules designed for that type of note, including modules designed for discovering missed revenue opportunities.
What happens when Charta detects coding or documentation errors? You decide: choose from direct autocorrect in your EHR, send automated notes to providers, or queue charts for human intervention.
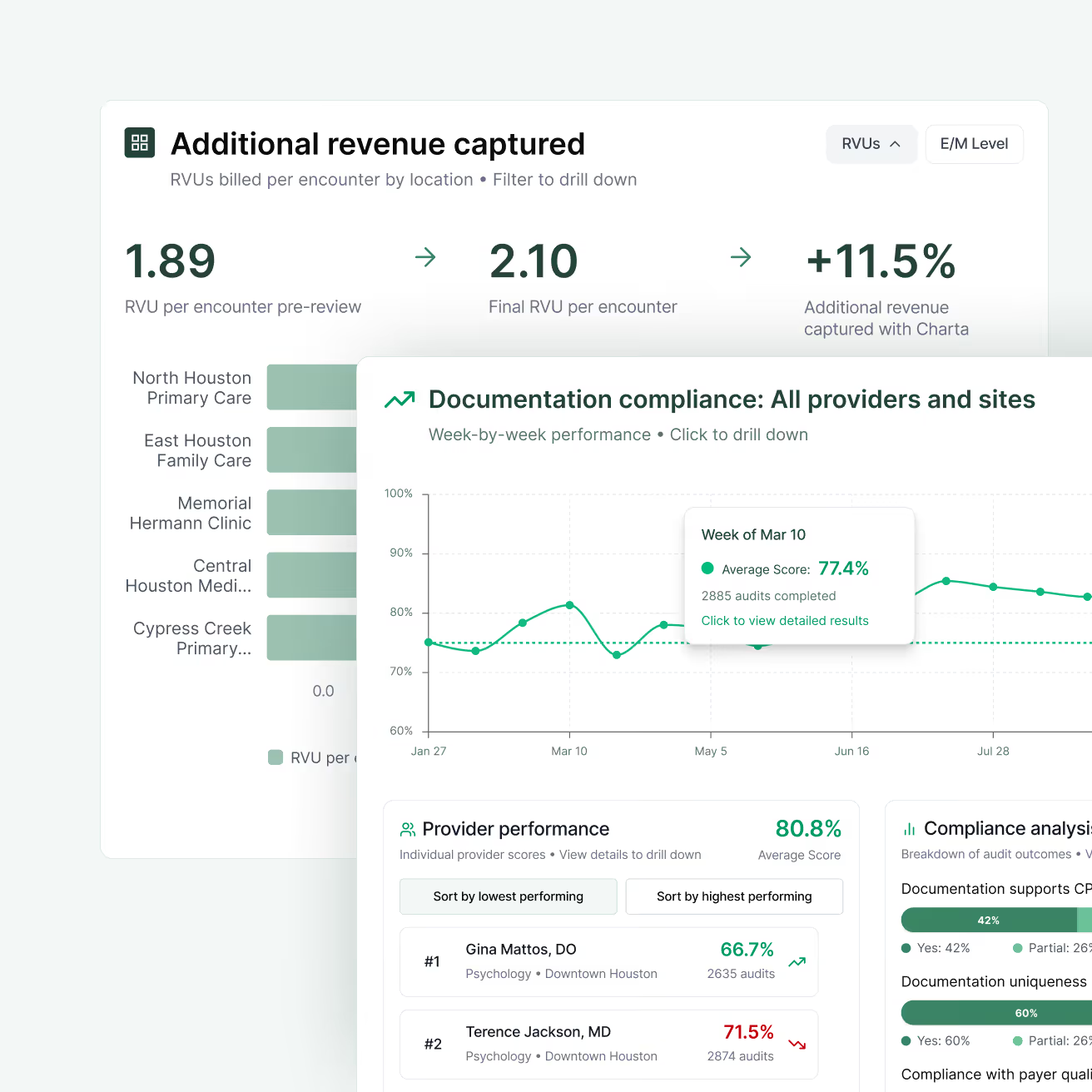
03. Detailed, real-time reporting
Following implementation, teams across your practice gain access to comprehensive data dashboards for tracking metrics related to revenue capture, clinical quality measures, and documentation compliance.
This shared source of truth across the practice will empower your team to raise revenue and clinical quality at the same time, leading to sustainable, long-term growth and always-on compliance assurance.
Resources
Browse our library of resources and tools to learn more about how AI chart review can unlock new efficiencies for your organization.









