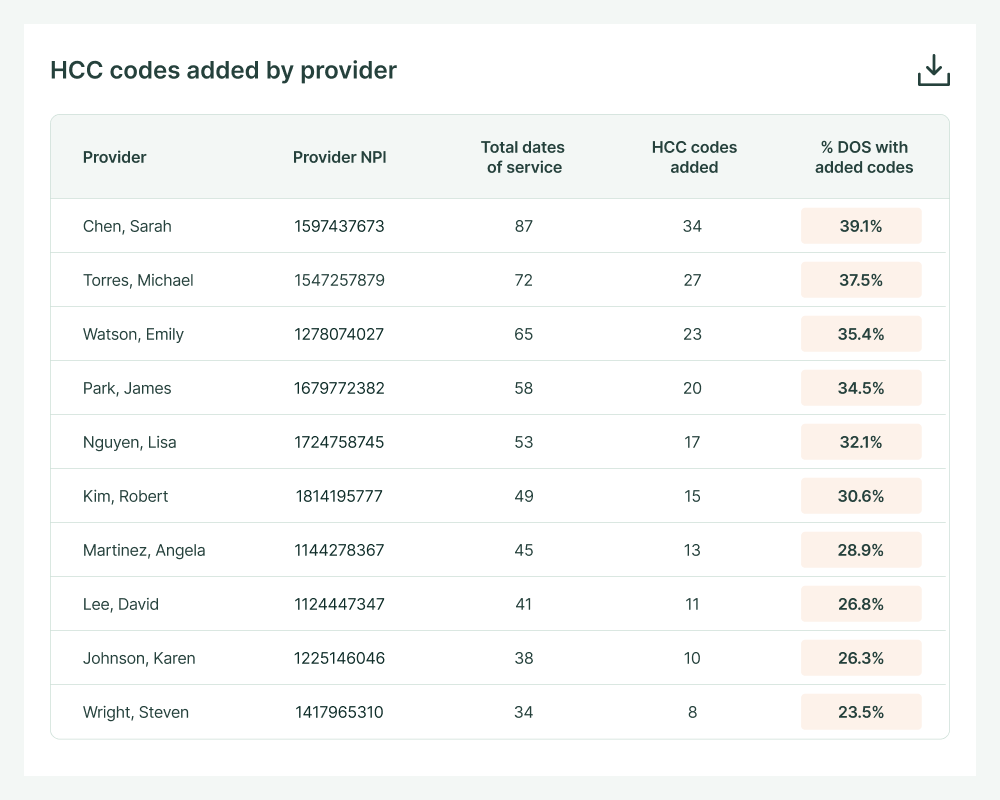
AI that delivers higher ROI and deeper insights for risk adjustment teams
Charta AI performs retrospective coding review with higher accuracy at a fraction of the cost of human coders and other tech-enabled solutions on the market.
Risk adjustment is stuck on legacy processes.
Expensive and time-consuming processes for retrospective HCC coding have long been the norm. AI brings new efficiencies and insights, including comprehensive data dashboards and more robust claims matching.
Higher accuracy at a fraction of the cost
Charta AI can read any type of documentation files, including scans and handwritten notes, to identify documentation that would support missing HCC codes.
+.0365
Net RAF improvement per member following first pass review ranges from 0.015-0.0365 with Charta.
29x
ROI on retrospective coding review with AI ranges from 12x to 29x.
Increase ROI on your retrospective chart reviews
See how one of the nation’s largest payers achieved 26x ROI by investing in AI chart review for retrospective coding.
More accurate HCC coding accuracy and clinical documentation integrity
In addition to our AI engine for retrospective coding analysis, Charta can flag records where documentation suggests prospective coding possibilities.
This content is updated in the Solutions CMS Collection.
Preview the true content by either 1.) going into preview (play button in the top right) and enabling custom code (switch in the top left) or 2.) publishing to staging and viewing there.
Fully coded notes, guaranteed
Ensure clinicians document and code every encounter at the highest defensible level. Charta identifies missed opportunities for accurate coding across your entire patient population, helping you receive fair reimbursement for complex care.
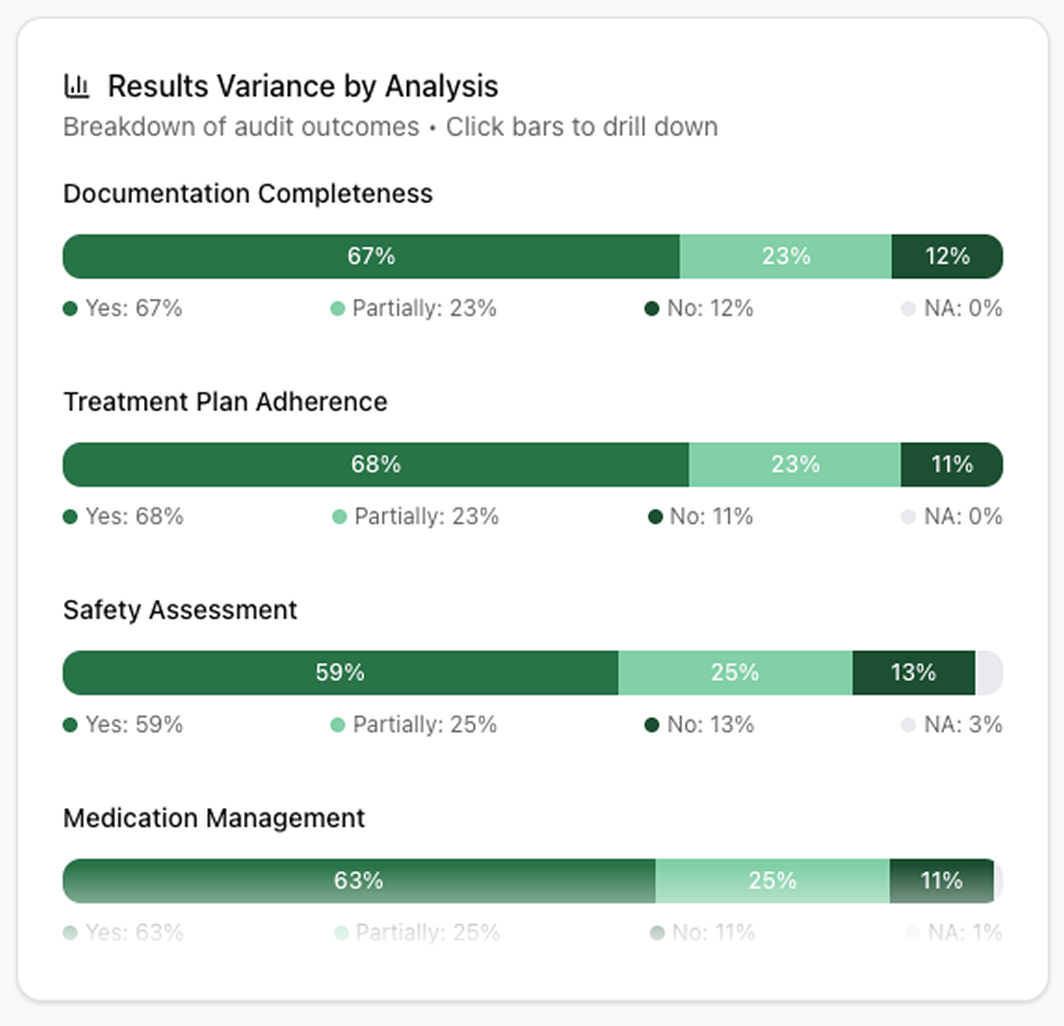
Get peace of mind and greater control
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, reducing denials and protecting your organization from payer audits.

Real-time provider feedback
Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.

More accurate HCC capture with less manual effort
Charta's AI analysis identifies potential diagnosis codes supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.

Autonomous coding
Instant, accurate codes for every encounter
Charta reviews all documentation immediately after note submission to completely and accurately code every service.
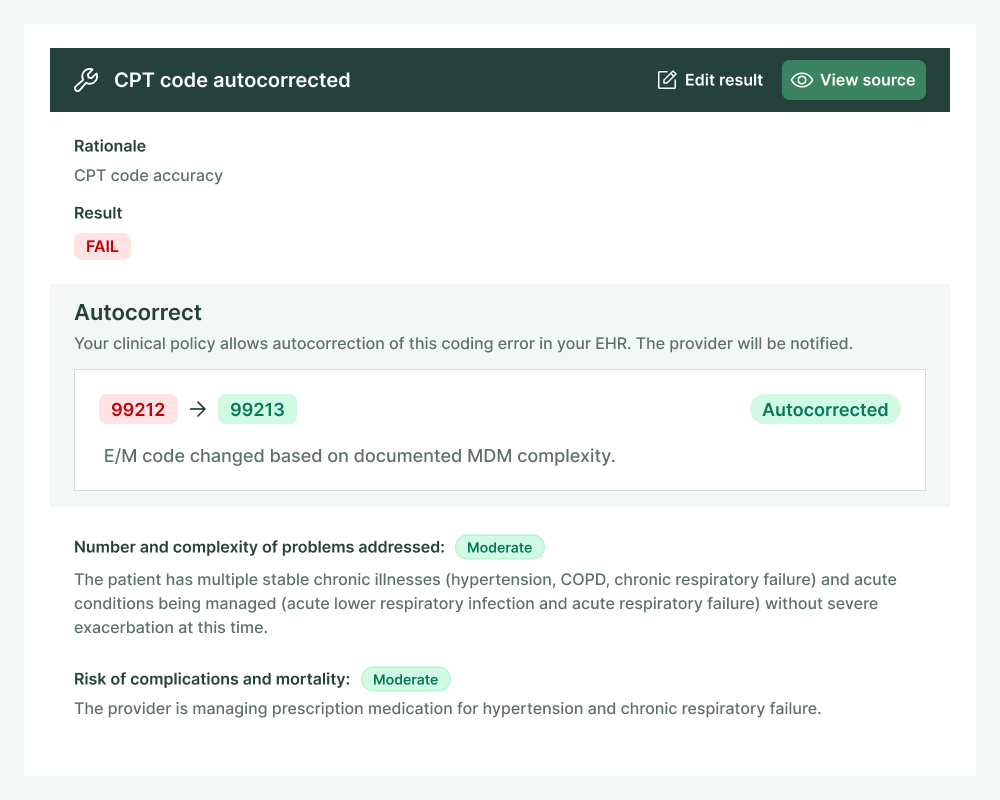
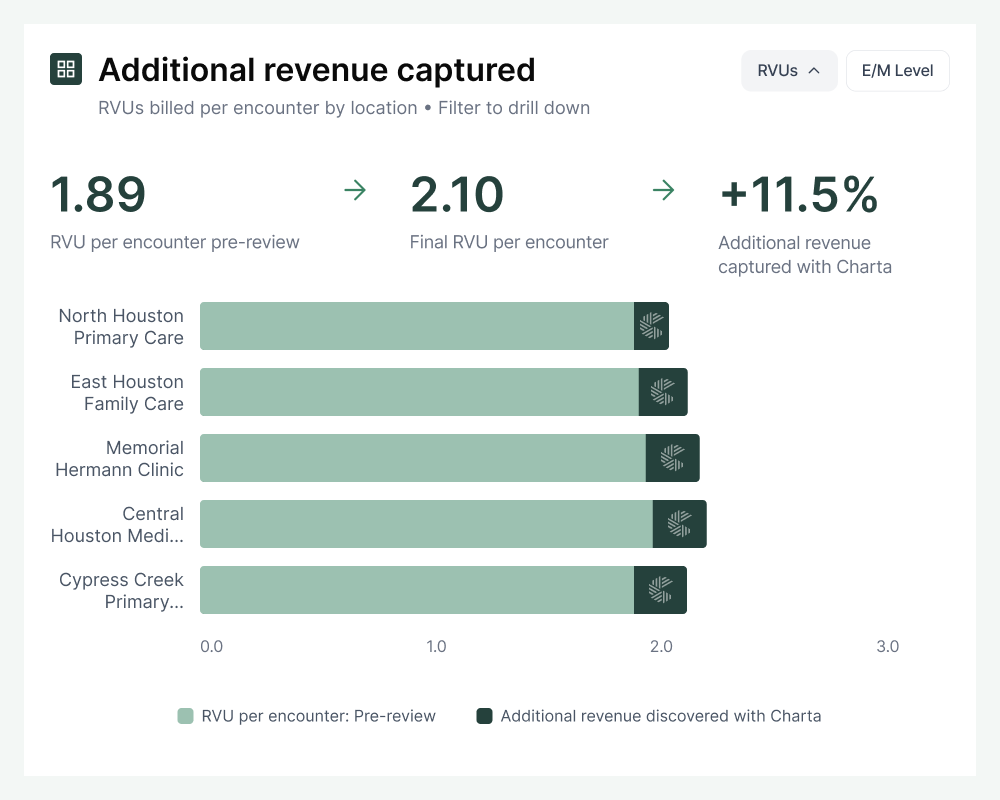
Revenue discovery
End coding-related revenue leaks
Charta detects and corrects missed revenue opportunities by ensuring you code every service delivered, and verifies that E/M codes are billed at the highest defensible level.
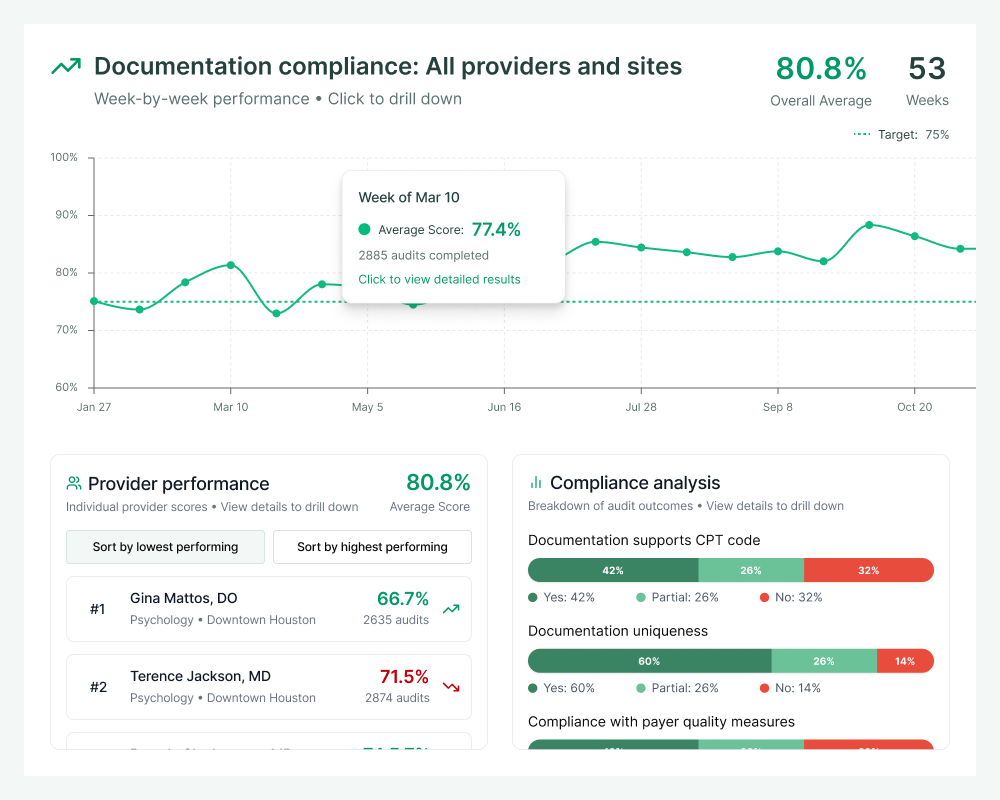
Payer compliance
Get peace of mind and greater control
By catching coding errors and documentation gaps pre-billing, Charta shifts your compliance strategy from reactive to proactive. Address issues while charts are still open, eliminating preventable denials and audit exposure.
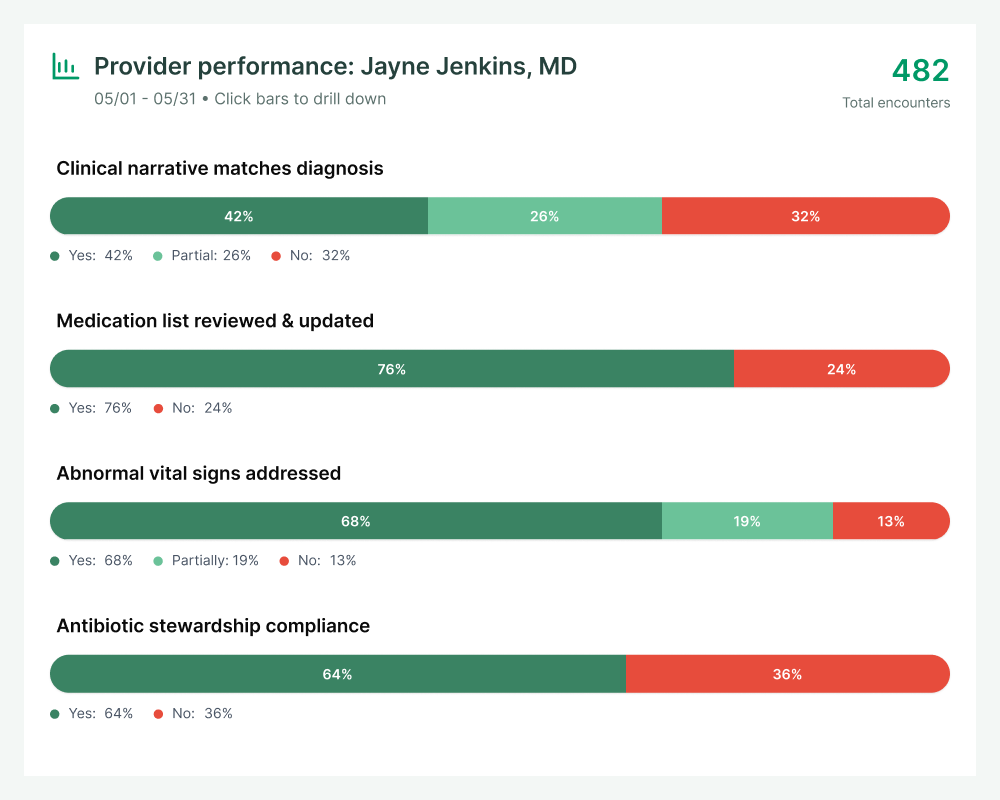
Clinical quality
Real-time provider feedback
Comprehensive analysis of every encounter gives clinical leaders actionable data on supporting quality measures, identifying care gaps and improving documentation quality. Automated feedback loops help providers improve in real-time, raising the quality of care and clinical records simultaneously.
Risk adjustment
Higher ROI and greater insights into risk adjustment
Charta's AI analysis identifies missed opportunities supported by clinical documentation, providing reviewers with direct citations to accelerate validation. The result: higher accuracy, faster turnaround, and reduced cost per chart reviewed.